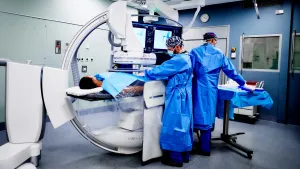
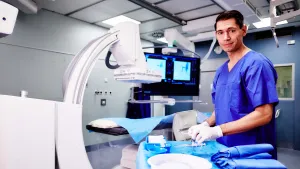
Our Interventional radiologists are board-certified physicians who specialize in minimally invasive, targeted treatments. They offer in-depth knowledge of the least invasive treatments available. They use X-rays, MRI and other imaging techniques to advance a catheter in the body, usually in an artery, to treat at the source of the disease non-surgically.
In our radiological care centers we offer a comprehensive spectrum of minimally invasive therapies. Our therapies are usually performed using local anesthesia.
CT-guided procedures.
- Pain therapy of the spine
Back pain is a widespread disease. A CT-guided back pain therapy is a gentle alternative to surgical procedures and allows targeted treatment of back pain. A typical epidural injection delivers two different medications into the space that surrounds the nerves emanating from the spine; the purpose of the injection is to provide temporary or prolonged relief from pain and inflammation. - CT-guided biopsies
In our hospital based Oncology Competence Centers we take CT-controlled tissue samples using local anaesthesia, which can be examined by a pathologist. In this way, the diagnosis is confirmed and examinations that enable targeted, individualized tumor therapy are carried out. - CT-guided drainage
Inflammations in the abdominal cavity cause so-called abscesses (pus cavities). With the aid of computed tomography, these inflammatory fluid accumulations can be precisely punctured. In many cases, this obviates the need for surgery.
Catheter-assisted interventions.
- Minimally invasive therapy of vascular diseases
Angioplasty: During angioplasty, using x-ray guidance, a catheter (i.e. a thin hollow tube) is passed through a blood vessel to the area of blockage. A balloon is inflated and breaks open the narrowing in the blood vessel. Depending on the severity and location of the blockage, an interventionalist might also place a stent (a tiny metal brace which keeps the artery open).
Thrombolysis: Thrombolysis treats acutely blocked arteries. This is usually an emergency treatment performed when the clot forms so quickly that the body has not time to grow new blood vessels to bypass the blockage. A thin tube is inserted through a tiny incision into a blood vessel and advanced to the blocked artery. A medication is delivered through the tube into the blood clot over 12-24 hours to dissolve it. The patient is hospitalized during the treatment. After the clot is dissolved, a patient may require additional treatments to open up any narrowed areas of the blood vessel. - Prostate Artery Embolisation in benign prostatic hyperplasia
While surgical procedures are standard practice for the management of benign prostatic hyperplasia (BPH), more and more patients and referring physicians are requesting a new procedure, Prostatic Artery Embolization (PAE), due to decreased recovery time, decreased pain, and decreased risk of sexual impairment. Using x-ray guidance, a small catheter is advanced through an artery in the groin into the blood vessel that supplies the prostate. Once identified, the blood vessel is occluded. Without nutrients and oxygen, the prostate shrinks. - Oncological Therapies
Transarterial chemoembolization (TACE) is used to treat e.g. certain types of inoperable primary liver cancer. Through a tiny hole in the groin or wrist, an interventionalist threads a catheter, thin tube, into the blood vessels supplying the liver tumor. The catheter delivers a high dose of a cancer-killing drug (chemotherapy) directly to the tumor. The chemotherapy is attached to small particles which then serve to block the artery, starving the tumor of its blood supply and preventing the chemotherapy from washing away and affecting normal healthy cells throughout the rest of the body. Chemoembolization usually involves a hospital stay of two to four days. Patients typically have lower than normal energy levels for about a month afterwards. Chemoembolization is a palliative, not a curative, treatment. - Transjugular Portosystemic Shunt (TIPSS)
The blood vessels which drain the intestines, the portal veins, empty into the liver. When the liver hardens due to cirrhosis, blood flow is obstructed and pressure builds in the portal vein like a kinked hose leading to bleeding and/or ascites (excess fluid in the abdomen). A TIPS acts as a bypass around the diseased liver. An interventionalist enters a blood vessel at the neck through a small incision, using x-rays, a catheter is guided through the blood vessel, through the heart, and into the liver. From there a needle is passed through the liver into the portal vein. Using that access, the interventionalist connects the portal vein to the hepatic vein which eventually drains into the heart, bypassing the diseased liver. Patients are kept in the hospital for a few days afterwards to assess the success of the complex treatment and be monitored for any complications. - Hemodialysis Access and AVF maintenance
When patients reach the final stage of Chronic Kidney Disease (CKD), End Stage Renal Disease (ESRD), they will require renal replacement therapy (i.e. dialysis). We are able to provide temporary hemodialysis catheter placement as well as maintain already established access points. An arteriovenous fistula is a surgically created connection between an artery and vein which “arterializes” the vein and creates enough blood flow in your vein to allow your blood to be circulated and filtered by a dialysis machine. If your AVF malfunctions or clots, a patient may not be able to receive adequate dialysis. We work with our referring nephrologists, dialysis centers, and patients to provide optimal surveillance. - Biliary Drainage
In the course of various benign and malignant diseases, the bile flow from the liver may be altered. Symptoms may include severe itching, yellowish color of the skin and disturbances of digestive organs. With the so-called PTCD (percutaneous transluminal cholangiodrainage) the bile flow is restored. - Other interventions
In addition to the above-mentioned procedures, we also perform many other minimally invasive procedures (e.g. port implantations, removal of foreign bodies, etc.). Contact us, we will be happy to advise you.